CURRENT STATUS OF SYSTEMS-BASED CARE IN THE UNITED STATES
Plan Enrollment
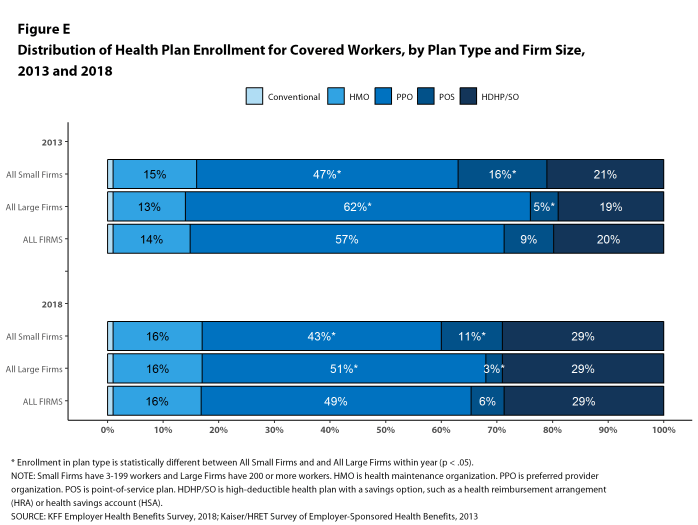
According to Henry J. Kaiser Family Foundation, Summary of Findings, “2018 Employer Health Benefits Survey” (October 3, 2018):
“PPOs continue to be the most common plan type, enrolling 49% of covered workers in 2018. Twenty-nine percent of covered workers are enrolled in a high-deductible plan with a savings option (HDHP/SO), 16% in an HMO, 6% in a POS plan, and less than one percent in a conventional (also known as an indemnity) plan [Figure E]. Covered workers in the South (55%) are more likely to be enrolled in PPOs than workers in other regions. Covered workers in the Midwest (39%) are more likely to be enrolled in HDHP/SOs than workers in other regions, while covered workers in the West (19%) are less likely to be enrolled in HDHP/SOs. The share of covered workers enrolled in POS plans decreased from 10% in 2017 to 6% this year.“
Why systems-based practice has grown in United States:
- Increasing costs of new medical technology
- Desire by employer groups to control increasing health care benefit costs
- Desire by employer groups to budget for health care coverage
HMO market has generally remained flat, while PPO market has jumped. If there is a choice, consumers are more likely to choose a PPO or point-of-service (POS) plan.
Growth of PPO Plans
Patients seem to want choice of providers and willing to pay a little more for that choice.
One reason systems-based practice continues to grow in the United States is because employers want to control increasing health care benefit costs. To control increasing health care costs corporate managers of these employer groups are developing partnerships among the employers, providers and insurance carriers.
Most health care benefits are paid for by an employer group prior to health care reform. Prior to managed care arrangements, the traditional health care insurance was indemnity type of coverage. Under indemnity coverage, the more services physicians render, more money physicians earn. Indemnity type of coverage allows free choice for patients of which physicians to go to and when.
Beginning in the 1980’s, corporate executives began to be concerned about health care costs growing out of control. There was basically no way of predicting health care costs from one year to the next. There was great uncertainty in budgeting for health care coverage for these companies employees. Costly new medical technology like MRI’s were increasing in use. The result was that the increased medical cost cut into the profit of these companies.
As a direct response to those concerns of the corporate buyers of health care, various insurance companies and managed care entities saw a marketing opportunity by offering solutions to help companies reduce health care expenses.
“A worker in company A breaks his arm. A worker in company B breaks his arm. Their breaks are identical. Why aren’t their medical bills?” – Wausau Insurance (advertisement)
Consider what many insurance companies are trying to sell to human resource and employee benefit directors and CEO’s of various companies. One of the common ways the insurance industry may try to sell managed care is by suggesting in its advertisements that “if you sign up with us to have us provide your health care insurance we can save you money.” An ad by Wausau Insurance in The Wall Street Journal for example reads: “A worker in company A breaks his arm. A worker in company B breaks his arm. Their breaks are identical. Why aren’t their medical bills?”
Another reason managed care continued to grow in the United States is because employers are insisting on accountability. This means employers want value in the health care products available and want to hold the partners accountable. Employers seek to contract with a selected group of providers who meet pre-defined cost, quality, and accountability criteria. Identifying program costs and outcomes are necessary to evaluate the cost benefits of corporate managed care programs. Comparing the outcomes with the predetermined goals or accountabilities of the program are necessary to assess the effectiveness of that program.
Employers want control over the health care services they are purchasing and in order to do that they hire these managed care organizations tomanage the health care delivery system that they are purchasing on behalf of their employees.
Paul Ellwood, the person who coined the term Health Maintenance Organization, does not think there’s any chance of the U.S. government taking over everything like in Medicare or the Canadian system, but that there is a high chance of the government “assuming greater financial responsibility for making sure that everyone has health insurance”.